MENU
JUMP TO
Learning About Police-Mental Health Collaboration Programs
To safely and effectively respond to people with mental illnesses, law enforcement agencies have relied upon Police-Mental Health Collaboration (PMHC) programs for 30 years. What started in a handful of agencies has expanded to thousands of agencies across the country. Effective PMHC programs are defined by collaborative partnerships with law enforcement agencies, mental health providers, and other community based entities. PMHC programs are producing better outcomes for consumers, officers, and agencies.
This section provides an overview of PMHC programs—the 10 essential elements of any PMHC, the various response strategies available to agencies, and the value that PMHC programs provide for law enforcement agencies, communities, and people with mental illnesses.
What is a Police-Mental Health Collaboration?
A PMHC is a law enforcement-based program that enables officers to respond appropriately and safely to people with mental illnesses. Mental health calls for service are among the most complex and time-consuming for law enforcement. PMHC programs allow officers to be safer, reduce repeat calls for service, minimize the strain on agency resources, and connect people with mental illnesses to services.
 | Take the PMHC Self-Assessment Tool and learn how to fully implement a PMHC. |
For More Information:
Benefits of Police-Mental Health Collaborations
PMHC programs can create positive changes for law enforcement agencies, law enforcement officers, communities, and consumers alike. Based on research and the experiences of agencies, the most common benefits are:
Improved Safety:
De-escalation strategies are a staple in all PMHC models and enable the trained officer to neutralize a situation without the use of force (or with the use of the least amount of force) that results in a decrease of injuries to both officers and consumers alike.
Fewer uses of force: Officers are less likely to use force, even in encounters considered as high violence risk. Additionally, when using force, they generally rely on low-lethality methods.
Fewer injuries to officers: Across the nation, police agencies are seeing a reduction in police officer injuries following the implementation of PMHC programs.
Fewer injuries to consumers: Officers are able to better understand and interpret crisis behavior and respond appropriately, which leads to fewer injuries to consumers.
Increased Access to Behavioral Healthcare:
Officers have a greater awareness of community resources allowing them to connect consumers to treatment, services, and other supports.
Increased use of crisis services: With an improved ability to identify mental health crisis, when appropriate, officers are more likely to divert individuals from the criminal justice system to crisis services.
More referrals to appropriate behavioral health services: PMHC officers become acquainted with mental health services in their community and more often provide a referral or even transport to treatment.
Increased continuity of healthcare: Police-mental health collaborations result in ongoing community-based treatment solutions that enable the individual to remain stable.
Decreased Repeat Encounters with the Criminal Justice System:
When individuals are connected to treatment, they are less likely to engage in unlawful or disruptive behaviors, and therefore have fewer contacts with law enforcement and the criminal justice system at large.
Fewer arrests: Individuals connected to mental health treatment by officers experience fewer subsequent arrests than individuals not connected to services.
More jail diversions: With the ability to identify individuals in mental health crisis and their awareness of healthcare resources, officers are more likely to transport the individual to appropriate services than jail or lockup.
Reduced Costs:
Improved safety, increased access to mental healthcare, and decreased repeat encounters with the criminal justice system have resulted in reduced costs to law enforcement agencies.
Fewer repeat calls for service (CFS): When individuals are connected to mental healthcare services, they are less likely to call 911 themselves or to be the subjects of repeat complaints.
Fewer SWAT call-outs: PMHC officers are able to de-escalate potentially violent situations without having to employ SWAT.
Reduction in civil lawsuits: The decline in use of force and injury reduces money spent on litigation.
Reduction in time spent on mental health calls: When diversion services or receiving centers are in place, officers are able to resume patrol duties in a significantly shorter time.
Improved Community Relations:
Police-mental health collaboration programs lead to improved relationships between law enforcement agencies and their local partners and citizens.
Additional Resources
People with Mental Illnesses and Family Members
People with lived experience of mental illness—both individuals and family members—are key partners in police-mental health collaborations. They have first-hand experiences with the challenges of the mental health and criminal justice systems, and unique perspectives about the treatment and supports needed for recovery. Community organizations representing individuals and family members affected by mental illness also have significant community support and can contribute education, training, policy review and problem-solving to your collaboration.
Learn More about Partnering with People with Mental Illness and Family Members
- Improving Crisis Response and Safety: Sgt. A.D. Reflects on Partnerships with People Living with Mental Illness, Families and Mental Health Providers
- Justin Volpe’s Story: “It Stays with You When Someone Treats You with Respect”
- Tami Smith’s Story: “I Was Always Seeking Out Help. No One Listened to Me.”
Types of PMHC Programs
This toolkit highlights five types of PMHC programs. There is no one “right” type. Agencies need to first assess their community’s needs and resources to determine which type of PMHC is most appropriate. The five approaches are not necessarily mutually exclusive. That is, some agencies incorporate elements of different approaches into their programs, such as relying upon CIT officers or generalists and augmenting them with co-responder or mobile crisis teams.
See the YouTube Terms of Service and Google Privacy Policy
Agency Experiences
CMPD Crisis Intervention Team (CIT)
Law Enforcement Officers are frequently front-line responders to persons in crisis with a serious mental illness. In an effort to better prepare officers to respond to these individuals, CMPD is training with the Crisis Intervention Team, CIT. CIT is a community-based collaboration between law enforcement, local National Alliance on Mental Illness (NAMI), mental health consumers, mental health providers, community colleges and law enforcement training centers. CMPD's finest are better equipped to serve our community by providing appropriate care, for a crisis involving persons with a mental illness. If you would like to learn more about mental illness, please call 704-365-3454 or go online.
For more information about Charlotte-Mecklenburg Police Department:
Program Overview
One Mind
This brand new One Mind Initiative includes the One Mind Campaign, which seeks to ensure successful interactions between police officers and people in crisis and/or with mental health issues or disorders. The One Mind Campaign focuses on uniting local communities, public safety organizations, and mental health organizations so that the three become "of one mind."
For more information about One Mind:
AGENCY WEBSITE
Home Safe
Thousands of American families with aging parents or developmentally disabled children cope on a daily basis with the very real fear that those family members may wander from caregivers’ supervision, sometimes with tragic results. To avoid these tragedies, the Bureau of Justice Assistance (BJA) provides funding to law enforcement and public safety agencies to implement technologies to track missing individuals and to develop or operate programs to prevent wandering, increase safety, and facilitate rescue.
Kevin and Avonte’s Law (H.R. 4221 and S. 2070), was named in honor of two boys with autism who wandered from safety and tragically lost their lives. Kevin and Avonte’s Law is aimed at helping families locate missing loved ones with Alzheimer’s disease, Autism and related conditions. The legislation supports initiatives that reduce the risk of injury or death of individuals with developmental disabilities, who due to their condition may wander from safe environments.
Kevin and Avonte’s Law authorized BJA's Reducing Injury and Death of Missing Individuals with Dementia and Developmental Disabilities Program.. This program will support local efforts to address this public safety challenge by providing grants to health care agencies, law enforcement and public safety agencies, and nonprofit organizations, that implement locative technologies to track missing individuals, and/or develop or operate programs to prevent wandering, increase individuals’ safety, and facilitate rescue. These efforts will promote education and training of caregivers to prevent wandering and provide law enforcement officers the tools they need to help recover missing loved ones.
The IACP serves as the training and technical assistance provider to grantees of BJA's Reducing Injury and Death of Missing Individuals with Dementia and Developmental Disabilities Program.
For more information visit:
Home Safe
The Essential Elements of PMHC Programs
For any type of PMHC program, there are 10 essential elements that, if implemented, will contribute to the program’s success. The essential elements are drawn from existing PMHC programs to ensure that they are practical and valuable, while allowing for differences in every jurisdiction’s needs and resources. Because the elements provide a common framework for program design and implementation, they can be used to build a new PMHC program or improve an existing program.
1. Collaborative Planning and Implementation
Organizations and individuals representing a wide range of disciplines and perspectives and with a strong interest in improving law enforcement encounters with people with mental illnesses work together in one or more groups to determine the response program’s characteristics and guide implementation efforts.
2. Program Design
The planning committee designs a specialized law enforcement-based program to address the root causes of the problems that are impeding improved responses to people with mental illnesses and makes the most of available resources.
3. Specialized Training
All law enforcement personnel who respond to incidents in which an individual’s mental illness appears to be a factor receive training to prepare for these encounters; those in specialized assignments receive more comprehensive training. Dispatchers, call takers, and other individuals in a support role receive training tailored to their needs.
4. Call-Taker and Dispatcher Protocols
Call takers and dispatchers identify critical information to direct calls to the appropriate responders, inform the law enforcement response, and record this information for analysis and as a reference for future calls for service.
5. Stabilization, Observation and Disposition
Specialized law enforcement responders de-escalate and observe the nature of incidents in which mental illness may be a factor using tactics focused on safety. Drawing on their understanding and knowledge of relevant laws and available resources, officers then determine the appropriate disposition.
6. Transportation and Custodial Transfer
Law enforcement responders transport and transfer custody of the person with a mental illness in a safe and sensitive manner that supports the individual’s efficient access to mental health services and the officers’ timely return to duty.
7. Information Exchange and Confidentiality
Law enforcement and mental health personnel have a well-designed procedure governing the release and exchange of information to facilitate necessary and appropriate communication while protecting the confidentiality of community members.
8. Treatment, Supports, and Services
Specialized law enforcement-based response programs connect individuals with mental illnesses to comprehensive and effective community-based treatment, supports, and services.
9. Organizational Support
The law enforcement agency’s policies, practices, and culture support the specialized response program and the personnel who further its goals.
10. Program Evaluation and Sustainability
Data are collected and analyzed to help demonstrate the impact of and inform modifications to the program. Support for the program is continuously cultivated in the community and the law enforcement agency.
Resources
Get the Facts - Behavioral Health Issues in Jails and Prisons PowerPoint Presentation
Forensic Assertive Community Treatment (FACT) Information Sheet
Protection and Advocacy Information
International Association of Chiefs of Police
CIT – It’s More than Just Training!
Statewide Implementation of the Crisis Intervention Team Program: The Ohio Model
FAQs
Learning
Law Enforcement-Mental Health Learning Sites
Support jurisdictions in exploring strategies to improve the outcomes of encounters between law enforcement and people who have mental illnesses.
Contact Police Mental Health Collaboration
Please submit questions, policies and training materials that can benefit others for review and consideration.
Focused Tools for Law Enforcement
Many communities struggle with the PMHC program design process. Communities are unsure how to design and develop a PMHC program that meets their distinct needs and challenges. One way to increase knowledge of PMHCs, is to review programs that other jurisdictions have developed and tailor those programs to your specific community needs.
Law Enforcement agencies interested in expanding their knowledge base, starting, or enhancing a PMHC, can contact The U.S. Department of Justice’s Bureau of Justice Assistance (BJA) or BJA’s Training and Technical Assistance (TTA) Provider. BJA supports these urban and rural police departments to act as host-sites to visiting law enforcement agencies and their mental health partners.
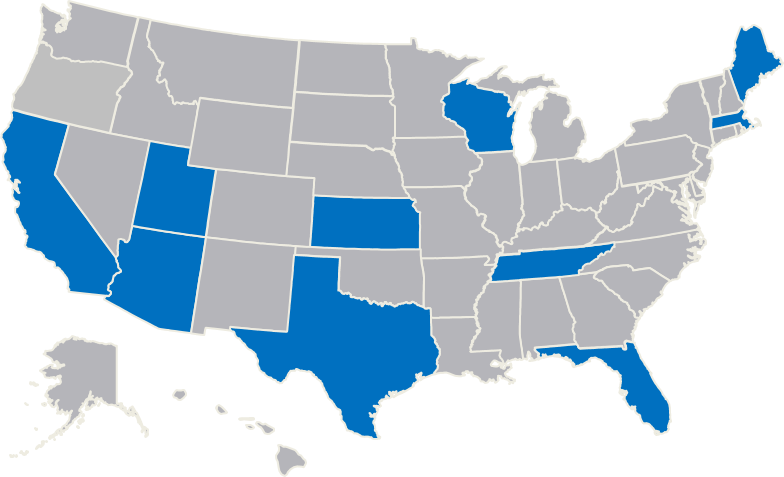
- Arlington (MA) Police Department
- Bexar County (TX) Sheriff's Office
- Harris County (TX) Sheriff's Department
- Houston (TX) Police Department
- Los Angeles (CA) Police Department
- Madison County (TN) Sheriff's Office
- Madison (WI) Police Department
- Miami-Dade County (FL) Police Department
- Portland (ME) Police Department
- Salt Lake City (UT) Police Department
- Tucson (AZ) Police Department
- University of Florida Police Department
- Wichita (KS) Police Department
- Yavapai County (AZ) Justice & Mental Health Coalition
Located across the country, these learning sites represent a diverse cross-section of perspectives and program examples and are dedicated to helping other jurisdictions improve their responses to people with mental illnesses.
Opportunities
The fourteen learning sites host site visits from interested colleagues and other local and state government officials, answer questions from the field, and work with BJA’s TTA provider to develop materials for practitioners and their community partners.
TTA is provided to law enforcement agencies and their community partners in an effort to assist with the development or implementation of PMHC strategies. Supplemental funds can be made available to agencies that are interested in visiting the learning sites. This is a focused approach intended to provide your agency with access to outstanding peer resources for police-mental health collaboration programs.
To request TTA and receive confirmation within 36 hours of your request
Complete the TA request form.
For questions not addressed by the Law Enforcement Mental Health Learning Site web page, contact [email protected]